Do you feel pain because you fear it? The case of fibromyalgia
If you type “Is fibromyalgia ...”, Google suggests “Is fibromyalgia real?” Doctors agree it is a “real” medical condition involving both physical and mental mechanisms. Current research highlights the importance of people’s expectancies about their symptoms.
Fibromyalgia: what is it exactly? Literally, it means pain in tissue and muscles, but it involves much more than experiencing pain; people often also suffer from anxiety, fatigue, cognitive problems, and depression. Worldwide, 2.7% of the population suffers from fibromyalgia, women nearly four times more often than men. Research is still trying to identify what triggers fibromyalgia, and what may cause symptoms to persist over time. This knowledge gap seems to be the reason for the common misunderstanding that fibromyalgia is “not a real disorder”. Fibromyalgia impacts sufferers’ daily life in the sense that it may make it harder for them to participate in physical and social activities. This makes fibromyalgia a challenging syndrome to live with, both physically and mentally.
Associations
To further improve the quality of life of people living with fibromyalgia, we need to understand if and how their pain is affected by, for instance, their thoughts and feelings about pain. Current research is looking into how symptoms of fibromyalgia influence the way people link – or in scientific terms ‘associate’ – their environmental context with pain. Let’s delve deeper into how these associations are formed, and how they could affect pain.
Pain or no pain
Most people can differentiate with certainty between contexts where they may generally experience pain – a dental appointment, for example – and contexts – such as dining in a restaurant – where pain is unlikely. This difference may be less clear in the case of fibromyalgia, as pain symptoms may occur even in neutral contexts. This may, in turn, increase the likelihood of a sufferer associating a neutral context, such as a restaurant, with “pain” rather than “no pain”. We know from the scientific literature that when we expect pain, we often feel anxious. Anxiety releases certain hormones that make it easier to feel pain. Experiencing pain in a certain context may cause a person to also expect pain in comparable future situations. This initiates the cycle in which expectations about pain lead to experiences of pain, which continuously keeps repeating and strengthening itself (see figure below). In short, pain-related fear associations learned in the past may shape future pain experiences.
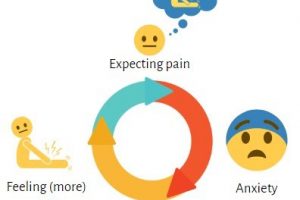
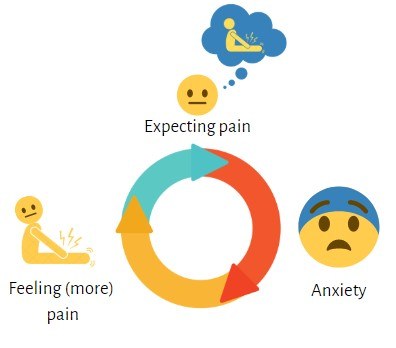
Safety cues
To investigate these learned associations, research has looked into how “safety” cues (cues that predict no pain; similar to the “neutral” situations mentioned before) may become a threat if another similar, but pain-related, cue is also present in the environment. In an experiment, groups of people with and without fibromyalgia were shown images of shapes (cues) on a computer. Following each image, participants received either a painful or non-painful sensation and reported how much pain and anxiety they felt. After a triangle was presented, participants always received a non-painful, cool sensation; after a square, on the other hand, they might receive either a painful hot or a non-painful cool sensation. Results of this study showed that the participants without fibromyalgia associated the triangle with ‘the absence of pain’ and were therefore able to identify this shape as a safety cue. However, in the group with fibromyalgia, higher levels of anxiety and pain were reported after the presentation of both the triangle and the square, indicating that they did not differentiate between the cues. A comparable study revealed that the fibromyalgia group did eventually learn to identify the safety cue, though they were slower at learning this than the control groups. However, this newly learned association was not transferred to other similar contexts. Overall, this suggests that fear of pain may more easily generalize to newer contexts in the case of people living with fibromyalgia.
Pain expectations
Preliminary research suggests that while people without fibromyalgia usually expect no pain in new situations, people with fibromyalgia may have to deliberately learn the new association that “this is not going to be painful”. We all know that once we have learned an association, it is difficult to learn to expect a different outcome. Imagine you have eaten some kind of food, let’s say shellfish. However, it turns out that the shellfish was bad, and you suffered from food poisoning. It will take you some time to learn that shellfish is safe to eat. Expectations and fear of pain seem to shape pain experiences in fibromyalgia, but further research is needed before we can draw firm conclusions about this.
Moving beyond skepticism
Currently, research is being conducted at Leiden University to shed light on the mechanisms behind the pain experiences in people with fibromyalgia. This knowledge can be used in the future to develop new treatment strategies to modify previously learned pain associations. Now that we are past the first stage of skepticism about the “reality” of fibromyalgia, the focus can shift to understanding how we can better identify this condition and optimize the interventions to improve the quality of life of people living with fibromyalgia.







